Medicare Advantage plans have long relied on retrospective chart reviews to ensure every diagnosis impacting a member's risk score is fully and accurately documented. But methods for patient risk adjustment through chart review are set to change.
In April 2025, CMS finalized a new rule related to code submissions. The rule will not take effect until calendar year 2027, but the health plans that adapt earliest will be the ones that come out ahead.
Unlinked chart review records
In its January 2026 Advance Notice for CY 2027, the Centers for Medicare and Medicaid (CMS) proposed one of the most consequential shifts to Medicare Advantage risk adjustment in years: the exclusion of diagnosis codes from unlinked chart review records (CRRs), starting in calendar year 2027. The agency finalized the change in its final rule for 2027 payment policies .
An unlinked chart review record (CRR) is a diagnosis code added to a member's risk adjustment submission as part of a retrospective medical record review, without any corresponding documented clinical encounter. This means that there is no corresponding record of a face-to-face visit or billable interaction where the diagnosis was assessed and managed during the applicable payer year.
Under the new rule, diagnoses surfaced through chart review alone—i.e., those that cannot be tied to a documented clinical encounter—will no longer count toward a member's risk score.
According to CMS, the rule change will reduce payments by approximately 1.53%—equivalent to a $7.2 billion drop in payments in 2027, compared with 2026.
Origins of the unlinked chart review record rule
For years, regulators and watchdogs have raised alarms about the way payers were using chart reviews to inflate risk scores without corresponding clinical evidence.
A 2019 HHS Office of Inspector General report estimated that unlinked chart review records generated $2.7 billion in potential overpayments in 2017, with MA payer organizations almost always using CRRs to add diagnoses rather than remove them.
More recently, CMS identified $7.5 billion in 2023 risk-adjustment payments tied solely to diagnoses that appeared in health risk assessments and nowhere else in the medical record.
The rule is also part of a broader, accelerating wave of scrutiny aimed at MA coding practices.
Learn more: Risk adjustment coding scrutiny is at an all-time high
Impact of the unlinked CRR rule
Revenue that was once attainable through retrospective review aimed at higher coding intensity will now need to be grounded in encounter-linked documentation from the outset. That means programs must now identify which diagnosis codes lack a qualifying clinical encounter and exclude them prior to submission.
Getting ahead of this rule isn't just about being prepared to comply with a new requirement. It's about building a risk adjustment program that is centered instead of the highest RAF accuracy. Plans that invest now in programmatically identifying diagnoses from unlinked charts will be better protected from the audit and enforcement risk that has become an unavoidable feature of operating in the Medicare Advantage market.
How Charta helps plans prepare for the rule
Charta uses advanced large language models (LLMs) to match charts to claims as the patient encounter data is ingested. LLMs can read and reason over documents of any file type, including handwritten notes, to parse the charts for crucial data to match them to claims, such as the date of service and the rendering provider’s name. This intelligent claims matching process results in systematic identification of claims without corresponding encounters that support the diagnosis.
Claims Intelligence Dashboard
The Claims Intelligence dashboard allows risk adjustment and Medicare Advantage program administrators to view key statistics about the review underway, including:
- Total charts received and processed by Charta
- Percentage total of the chase list those charts represent
- Total members represented by charts and claims data
- Total unique encounters analyzed
- Total unique claims reviewed
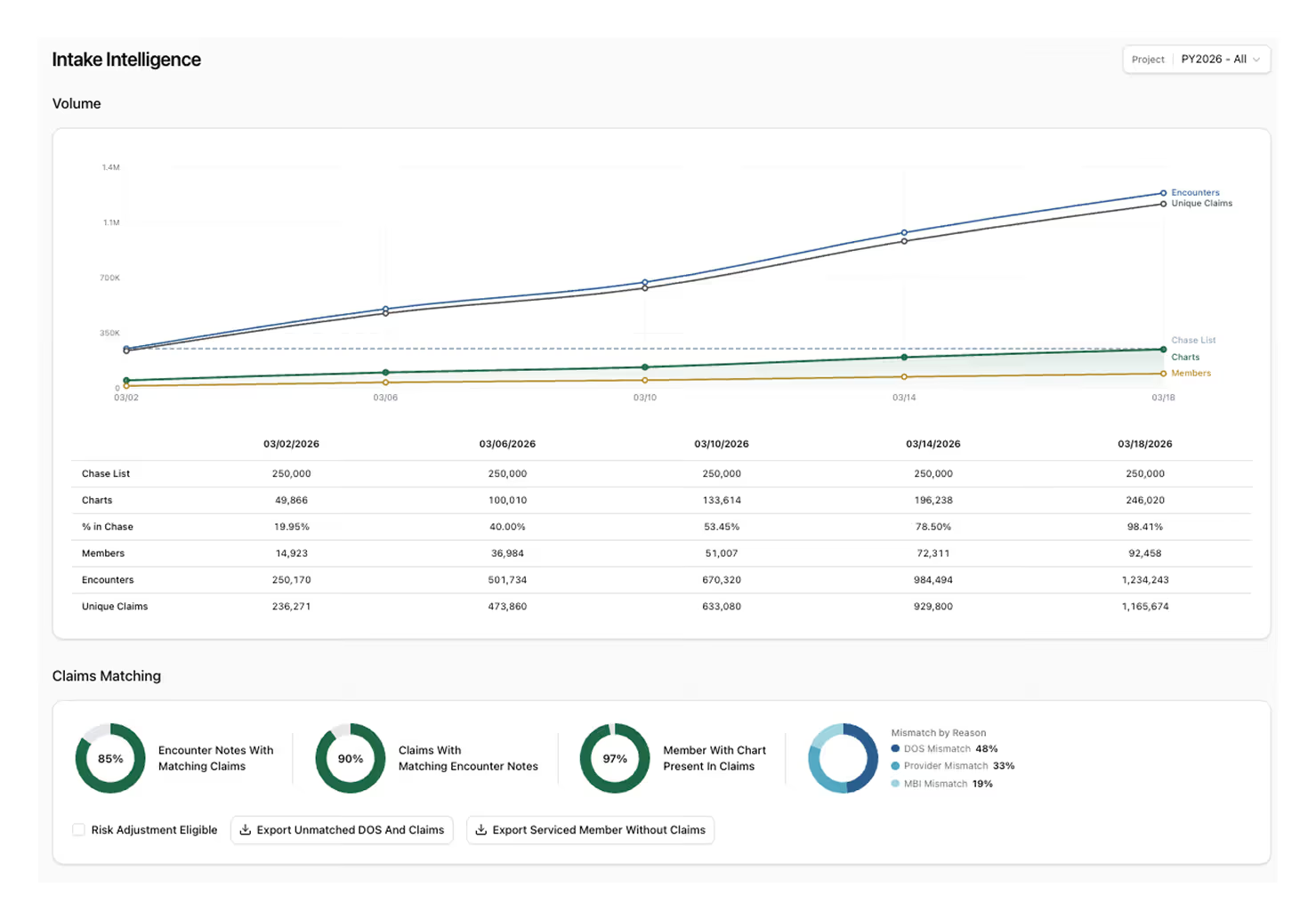
The Claims Matching gauges on the dashboard allow your team to understand at a glance which claims still lack a corresponding encounter, so you can focus your chase on the charts that matter most. In addition, the dashboard also tracks match rates by practice and provider, as well as high-risk HCC codes by prevalence.
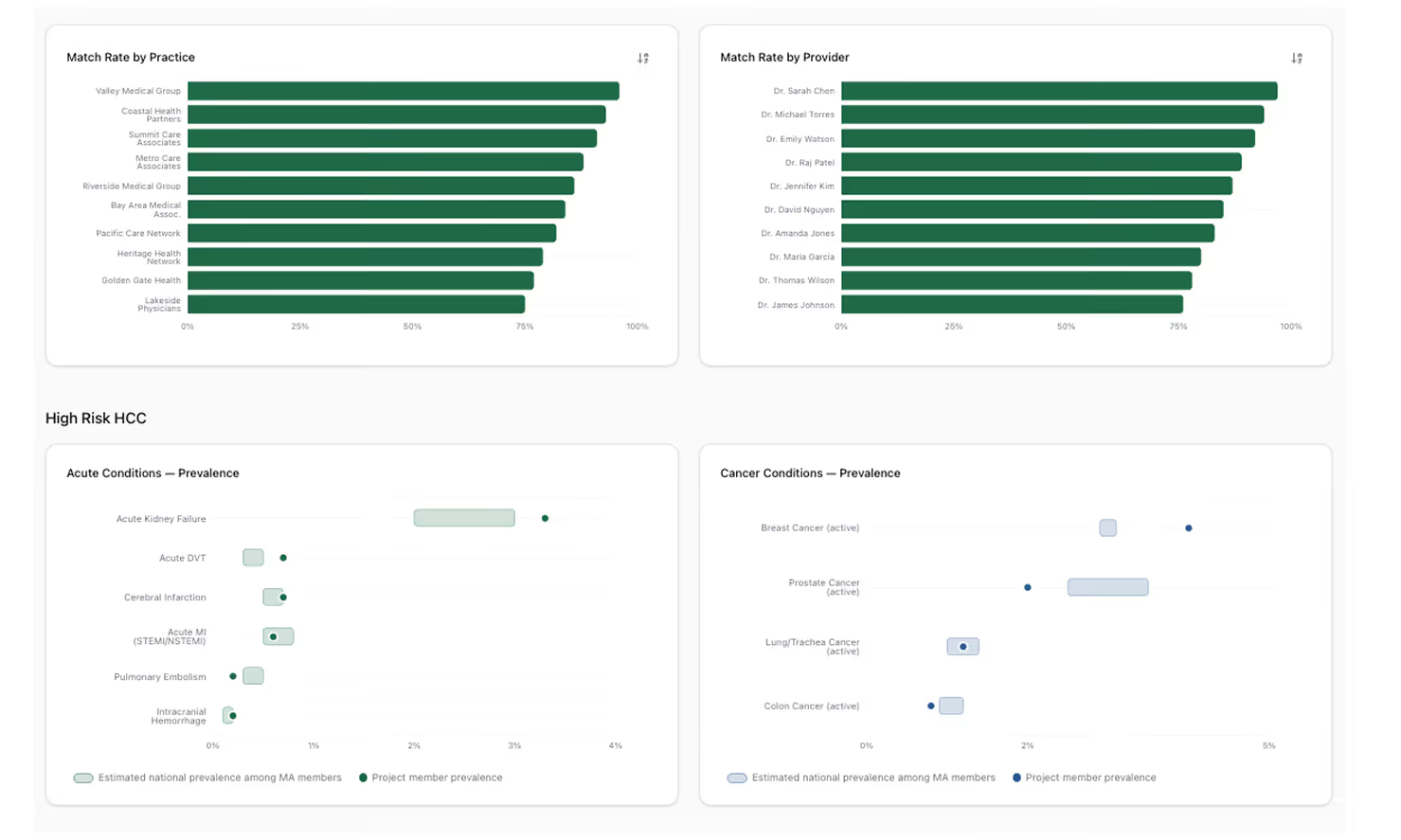
Bottom: High-risk HCC codes by prevalence
Gaining access to this information during intake helps your team understand where your claims data deviates from statistical norms.
Learn more
To learn more about how Charta helps risk adjustment teams stay ahead of the unliked chart review records rule change and achieve higher RAF accuracy at lower costs, reach out to schedule a demo from a member of our team today.