Automate chart review for teams across the practice
One unified platform for AI chart review replaces the tangle of point solutions fragmenting your back office—cutting tool costs, reducing complexity, and delivering on the efficiency gains that healthcare technology has long promised.
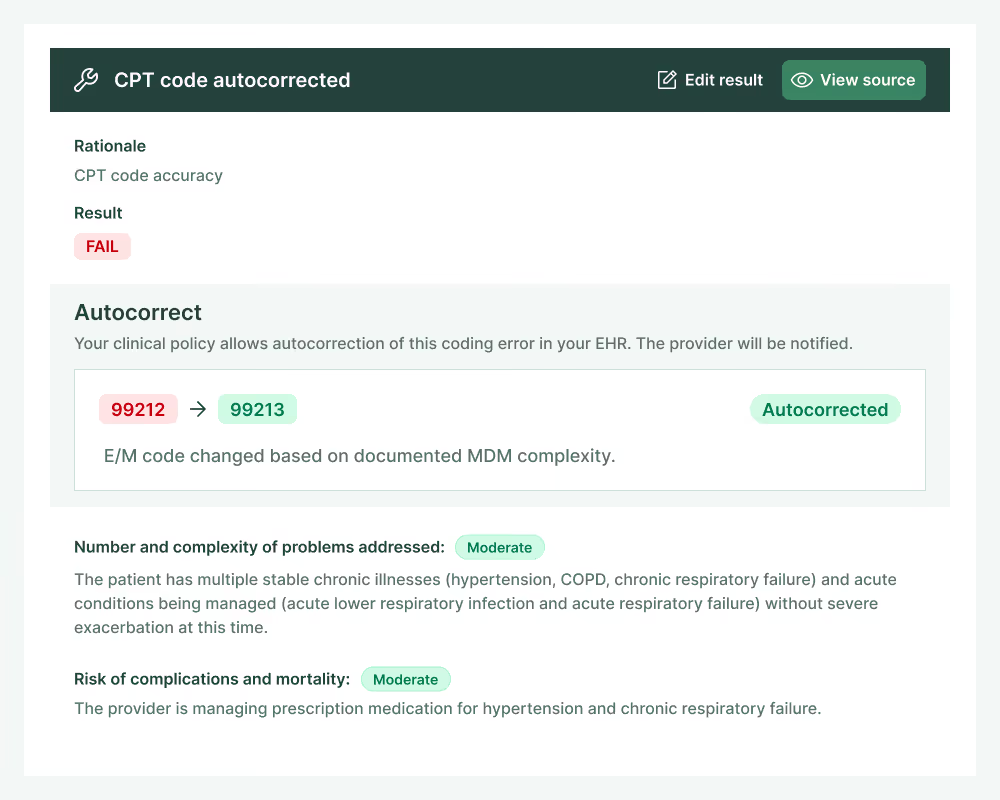
Autonomous coding
End revenue leak caused by coding errors with AI that fully codes every note based on provider documentation.
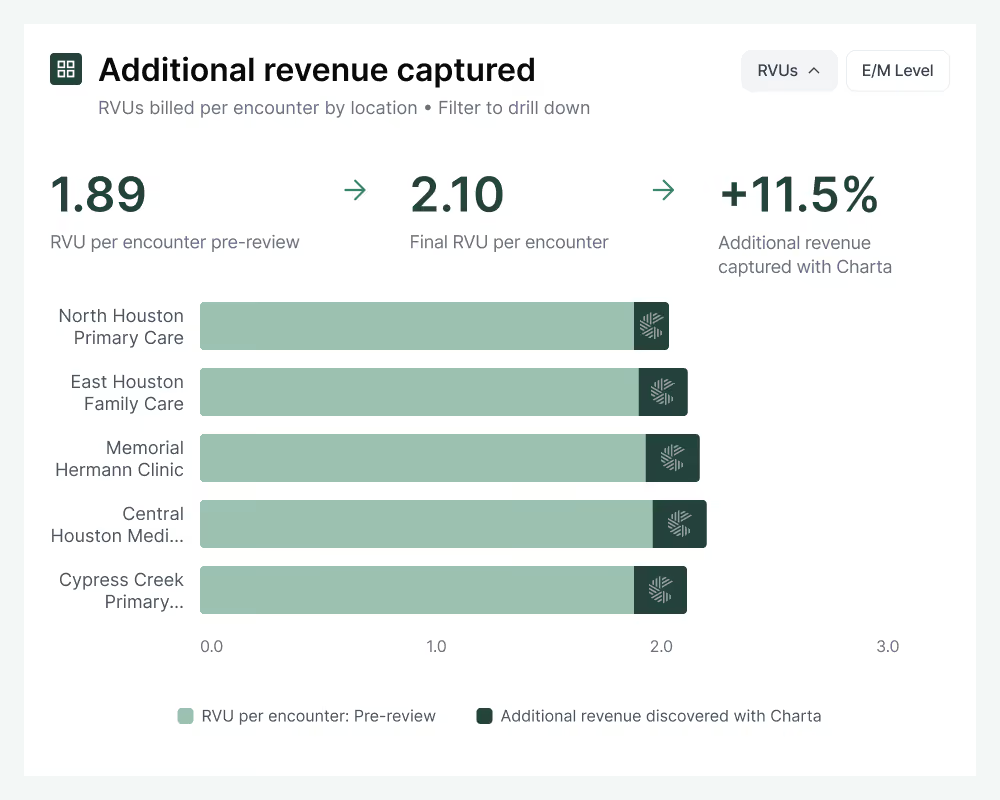
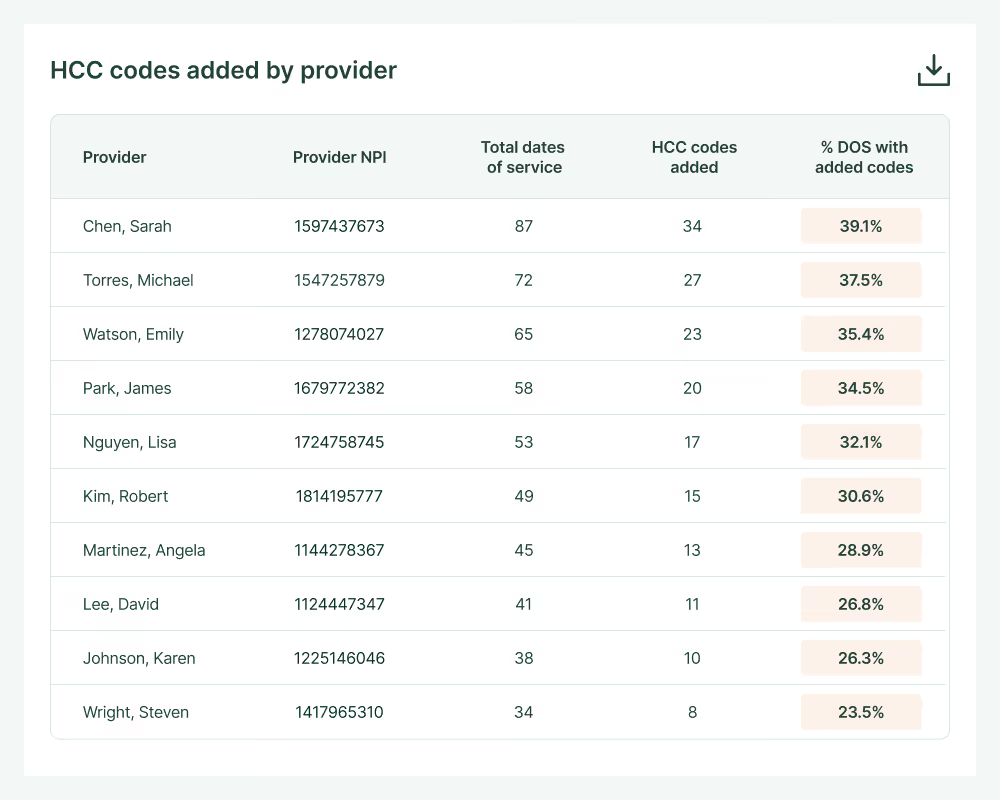
Revenue discovery
Automatically find and fix missed revenue opportunities before notes go to billing, across every chart.
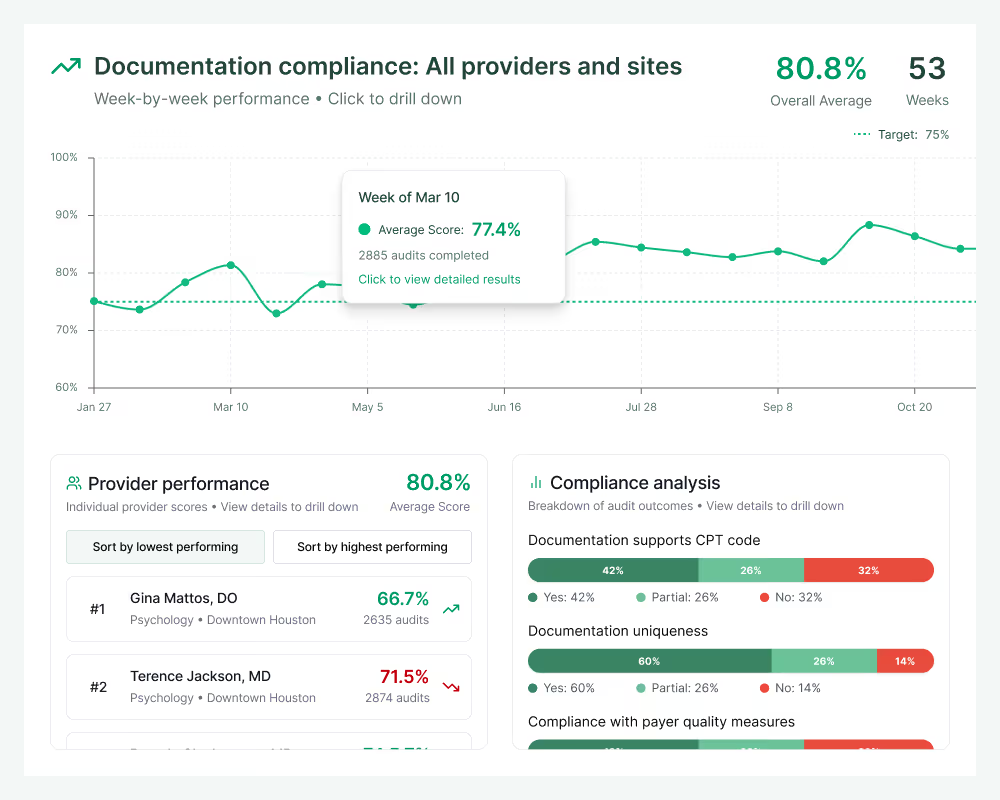
Payer compliance
Shift from risk mitigation to risk avoidance by having AI review every chart for pre-billing payer and regulatory compliance.
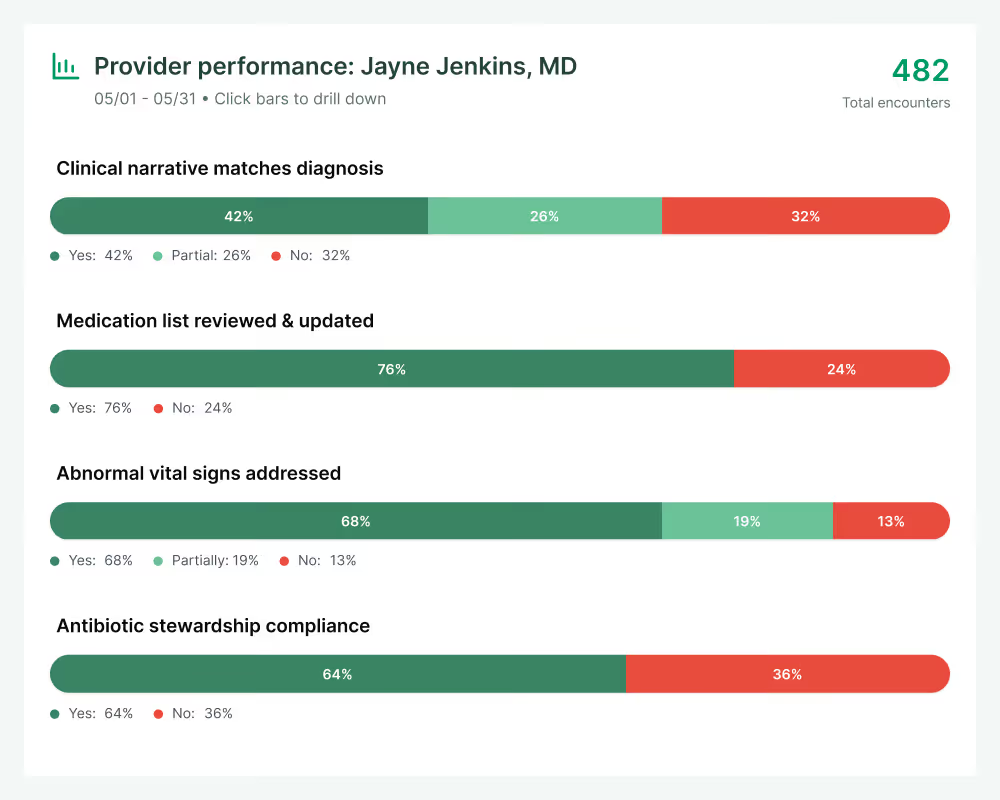
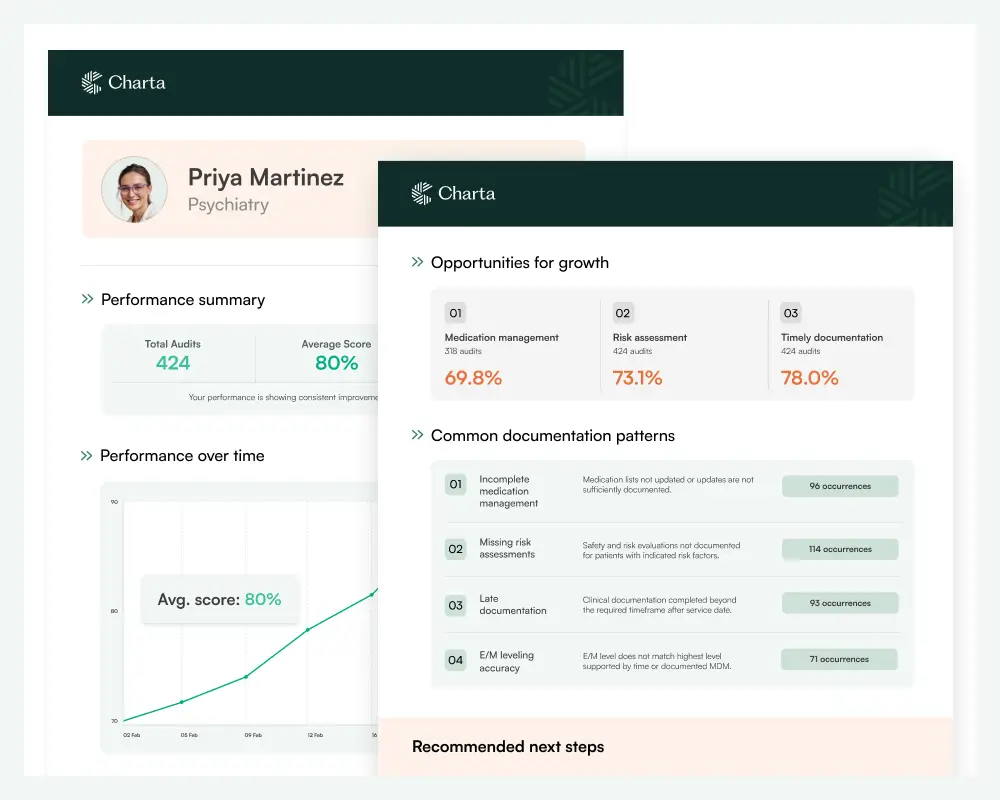
Clinical quality
Extend clinical reviews across 100% of patient encounters and gain real-time data insights across any set of clinical quality measures you want to track.
Resources
Browse our library of resources and tools to learn more about how AI chart review can unlock new efficiencies for your organization.