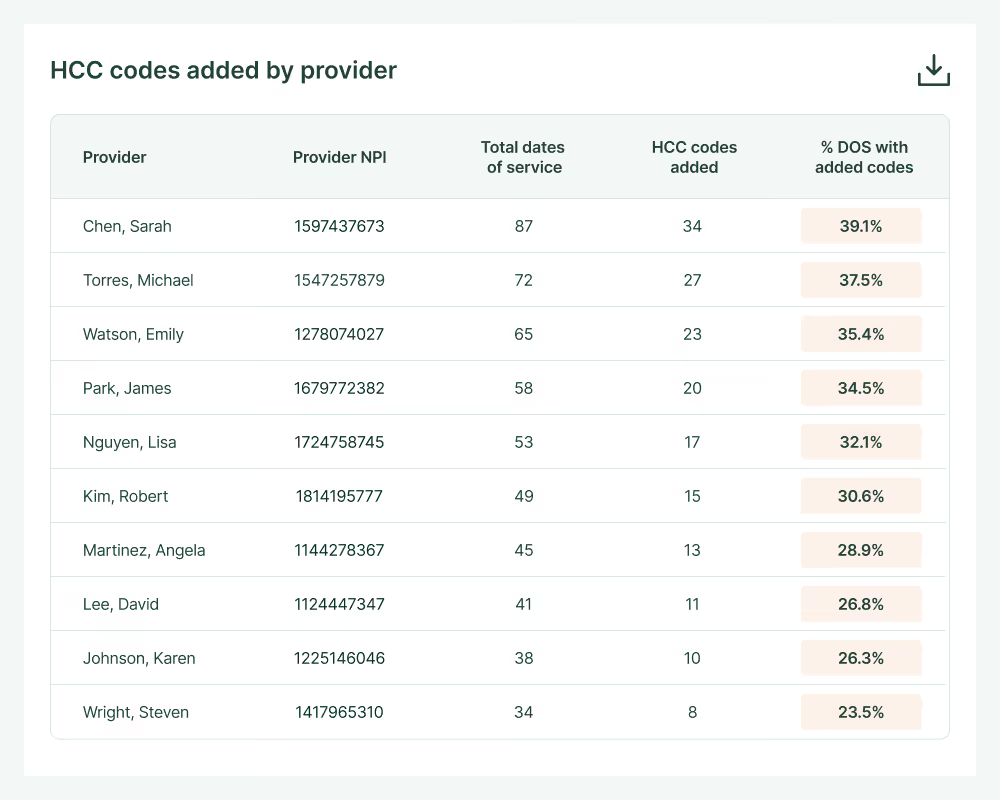
AI chart review built for modern health systems.
Charta builds custom AI chart review modules that help hospital health systems capture accurate and complete documentation across multiple specialties and payment models, whether fee-for-service, value-based care, or both.
Clinical documentation integrity can be achieved at scale with AI.
Modern health systems running both fee-for-service and value-based care face documentation complexity that costs them revenue, burdens their staff, and burns out their providers. Charta cuts through the complexity with AI chart review customized for complex health systems.
Close the gap between revenue earned and revenue captured
By reviewing every chart submitted for complete charge capture along with documentation compliance and clinical quality, Charta helps hospital systems close revenue and care gaps simultaneously.
13%
Percentage of revenue loss attributed to coding errors
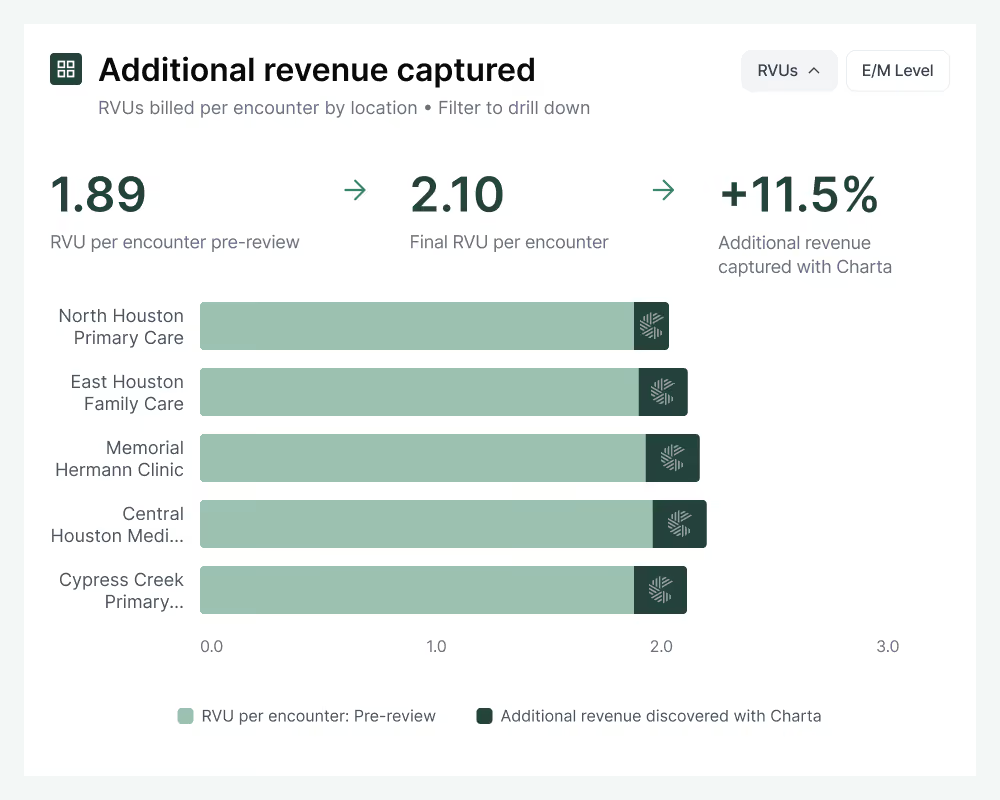
11%
Increase in RVU per encounter with AI chart review
Learn more about AI chart review
AI chart review enables health systems to create scalable systems for clinical documentation improvement for increased compliance and revenue capture.
Strengthen coding accuracy, documentation compliance, and clinical quality
Charta’s AI engineers customize every Charta integration to achieve the unique workflows of every health system we serve. Maximize revenue while raising the bar on documentation integrity and care delivery.
Instant, accurate codes for every encounter
Charta reviews all documentation immediately after note submission to completely and accurately code every service.
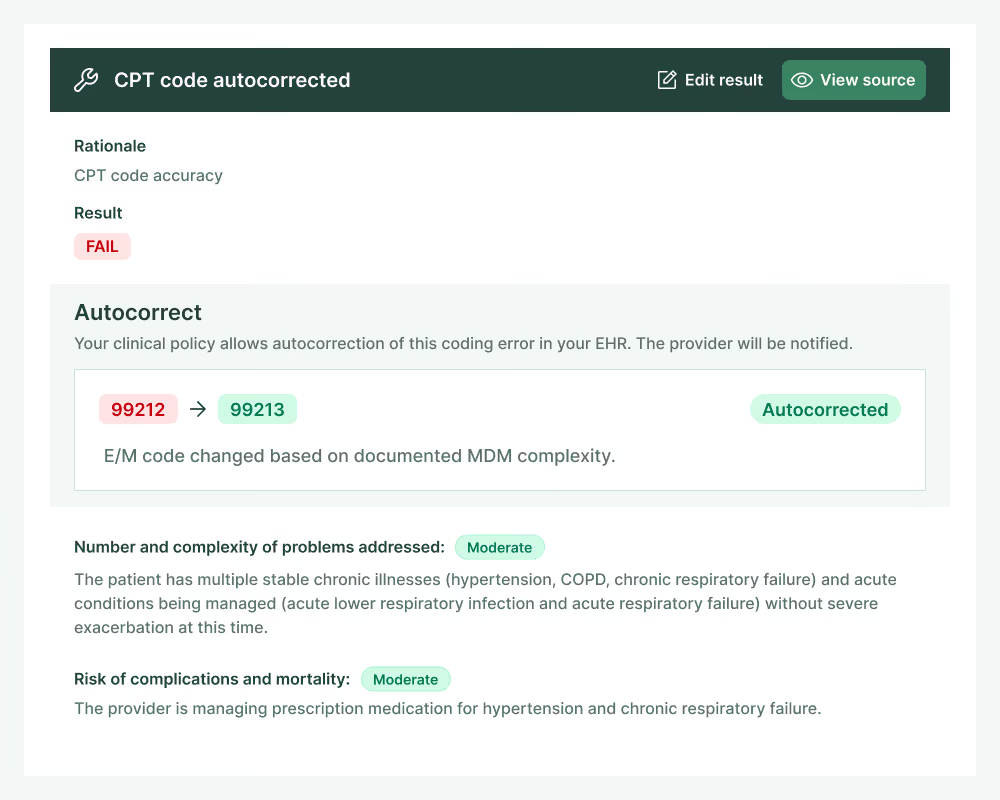
End coding-related revenue leaks
Charta detects and corrects missed revenue opportunities by ensuring you code every service delivered, and verifies that E/M codes are billed at the highest defensible level.

Get peace of mind and greater control
By catching coding errors and documentation gaps pre-billing, Charta shifts your compliance strategy from reactive to proactive. Address issues while charts are still open, eliminating preventable denials and audit exposure.

Real-time provider feedback
Comprehensive analysis of every encounter gives clinical leaders actionable data on supporting quality measures, identifying care gaps and improving documentation quality. Automated feedback loops help providers improve in real-time, raising the quality of care and clinical records simultaneously.

Higher ROI and greater insights into risk adjustment
Charta's AI analysis identifies missed opportunities supported by clinical documentation, providing reviewers with direct citations to accelerate validation. The result: higher accuracy, faster turnaround, and reduced cost per chart reviewed.

Autonomous coding
Instant, accurate codes for every encounter
Charta reviews all documentation immediately after note submission to completely and accurately code every service.
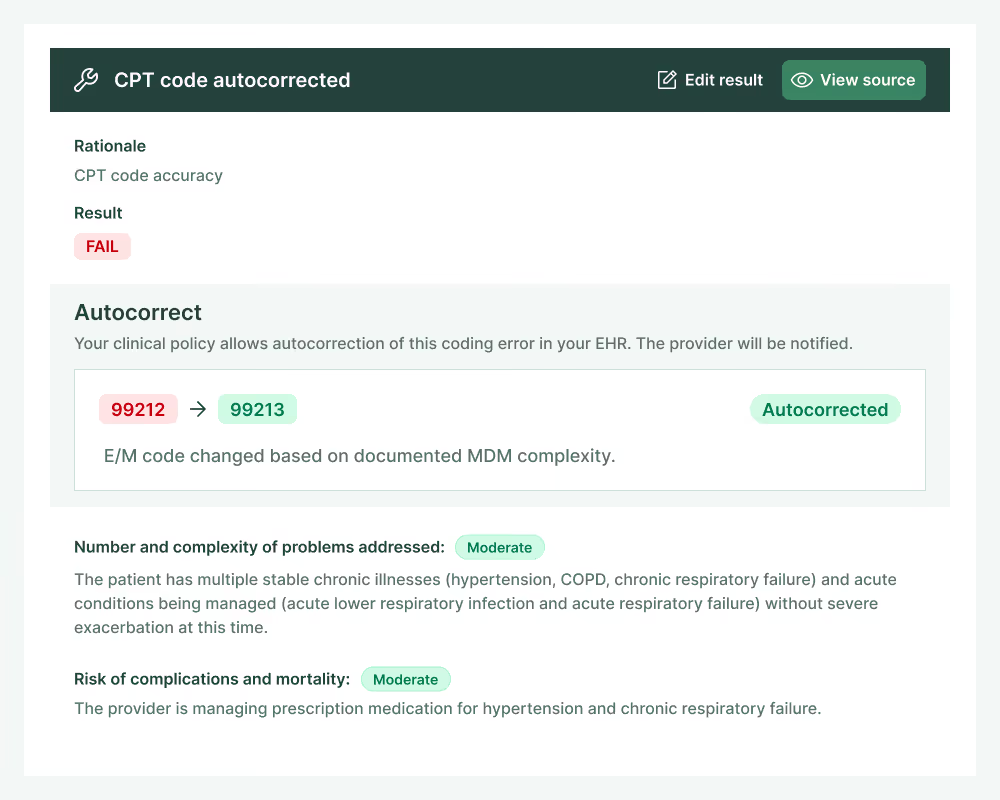
Revenue discovery
End coding-related revenue leaks
Charta detects and corrects missed revenue opportunities by ensuring you code every service delivered, and verifies that E/M codes are billed at the highest defensible level.
Payer compliance
Get peace of mind and greater control
By catching coding errors and documentation gaps pre-billing, Charta shifts your compliance strategy from reactive to proactive. Address issues while charts are still open, eliminating preventable denials and audit exposure.
Clinical quality
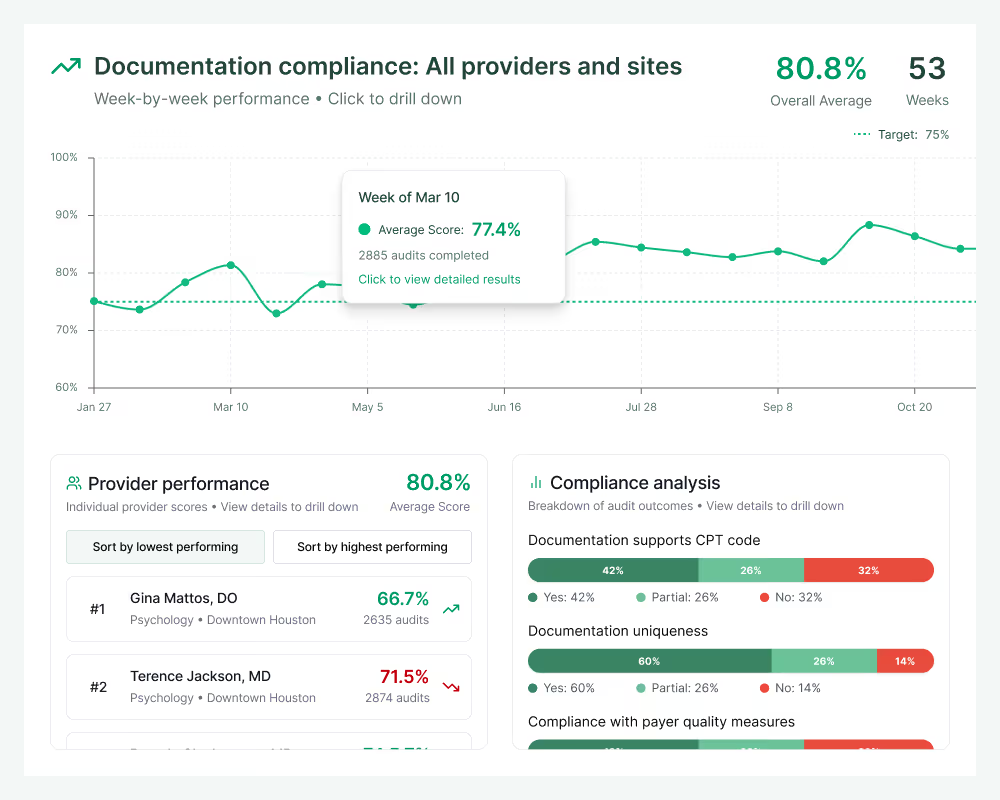
Real-time provider feedback
Comprehensive analysis of every encounter gives clinical leaders actionable data on supporting quality measures, identifying care gaps and improving documentation quality. Automated feedback loops help providers improve in real-time, raising the quality of care and clinical records simultaneously.
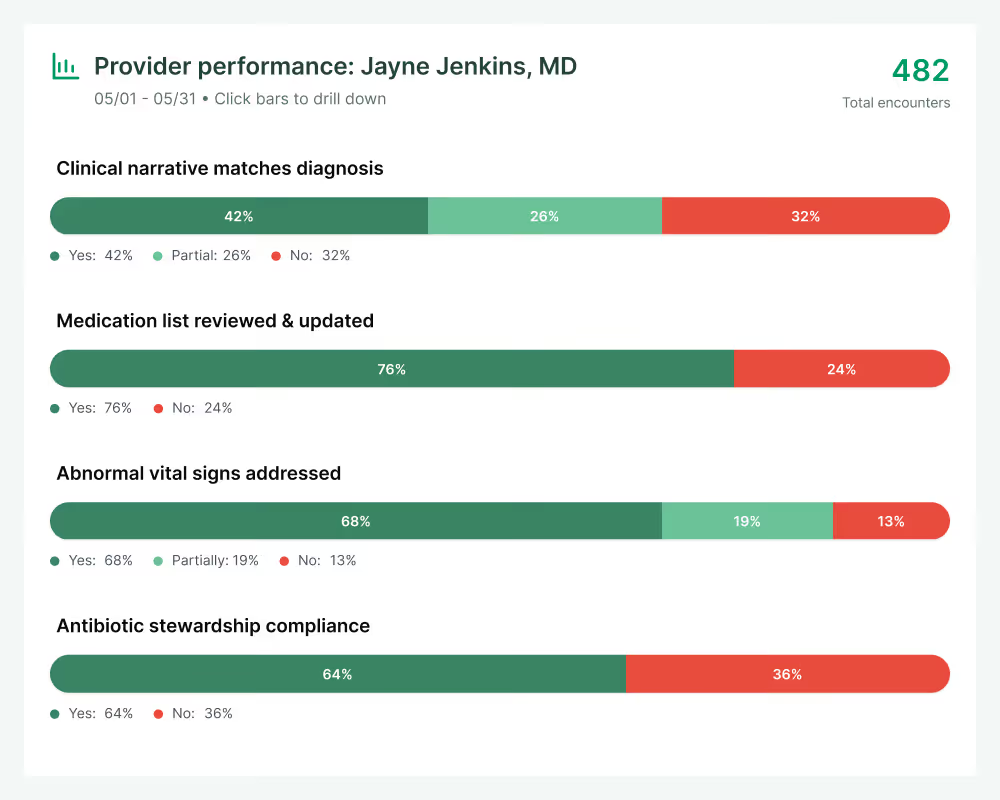
Risk adjustment
Higher ROI and greater insights into risk adjustment
Charta's AI analysis identifies missed opportunities supported by clinical documentation, providing reviewers with direct citations to accelerate validation. The result: higher accuracy, faster turnaround, and reduced cost per chart reviewed.