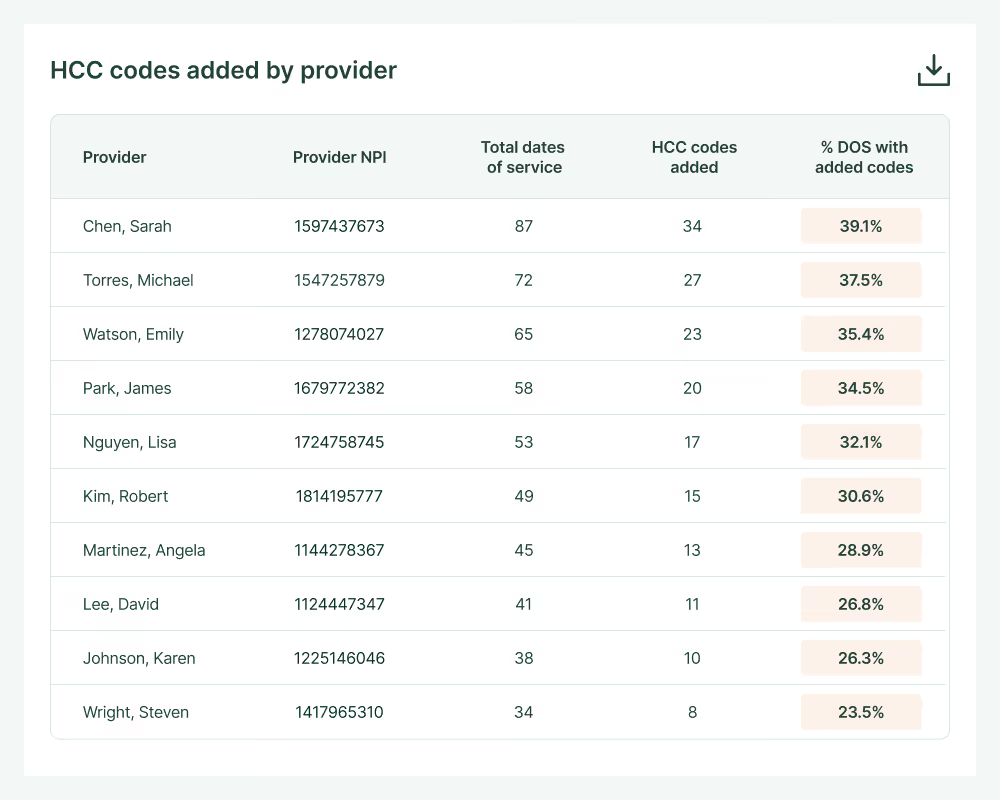
Ensure every chart meets payer standards
Charta reviews every chart immediately post encounter to ensure documentation adequately supports codes billed and meets payer-specific guidelines.
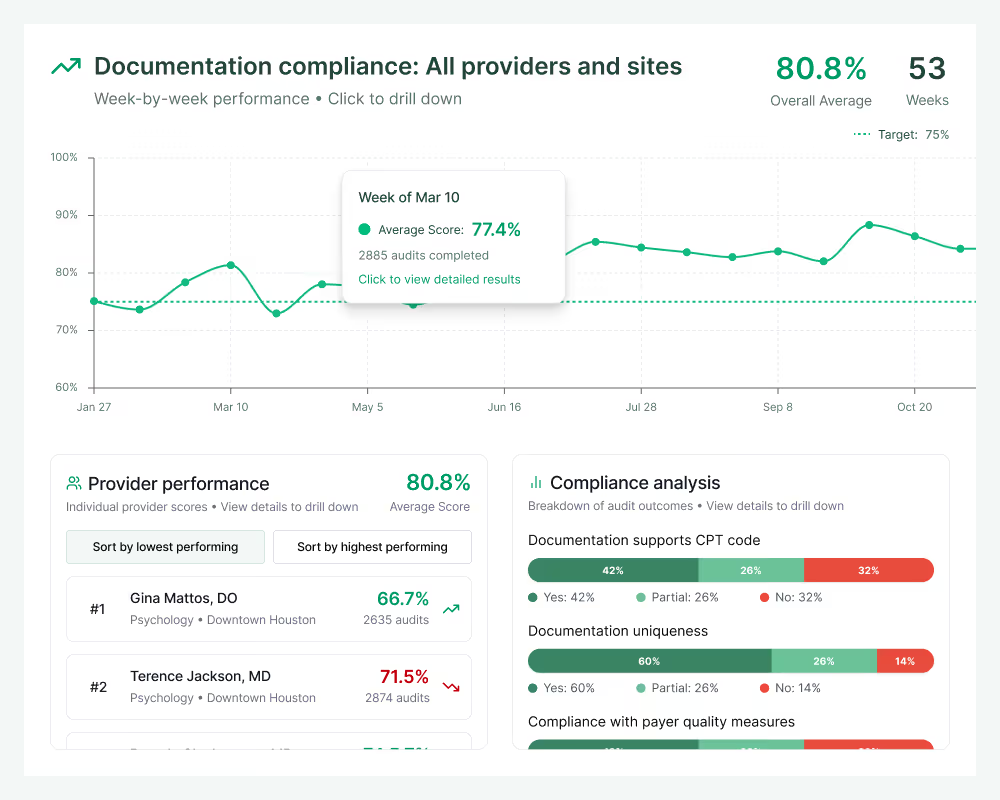
Charta reviews every chart immediately post encounter to ensure documentation adequately supports codes billed and meets payer-specific guidelines.

Traditional RCM compliance tools can typically only evaluate whether documentation is present, not whether it satisfies payer guidelines. AI has changed that. Charta conducts instant AI chart review for documentation compliance across specialities and payers.
Charta conducts sophisticated analysis on every chart to confirm that billing codes are fully supported by provider documentation. Charta can read and interpret any document type, including handwritten notes, to assess charts for uniqueness, completeness, and payer compliance. With Charta, you'll guarantee payer compliance at the pre-billing stage.
Charta enables 100% pre-billing payer compliance across every patient encounter.
Reduction in documentation compliance risk.
Charta’s AI decisions are backed by detailed reasoning and document citations, meaning you’re always be prepared for an audit, even as you reduce risk exposure.
By catching coding errors and documentation gaps pre-billing, Charta shifts your compliance strategy from reactive to proactive. Address issues while charts are still open, eliminating preventable denials and audit exposure.
Charta reviews all documentation immediately after note submission to completely and accurately code every service.
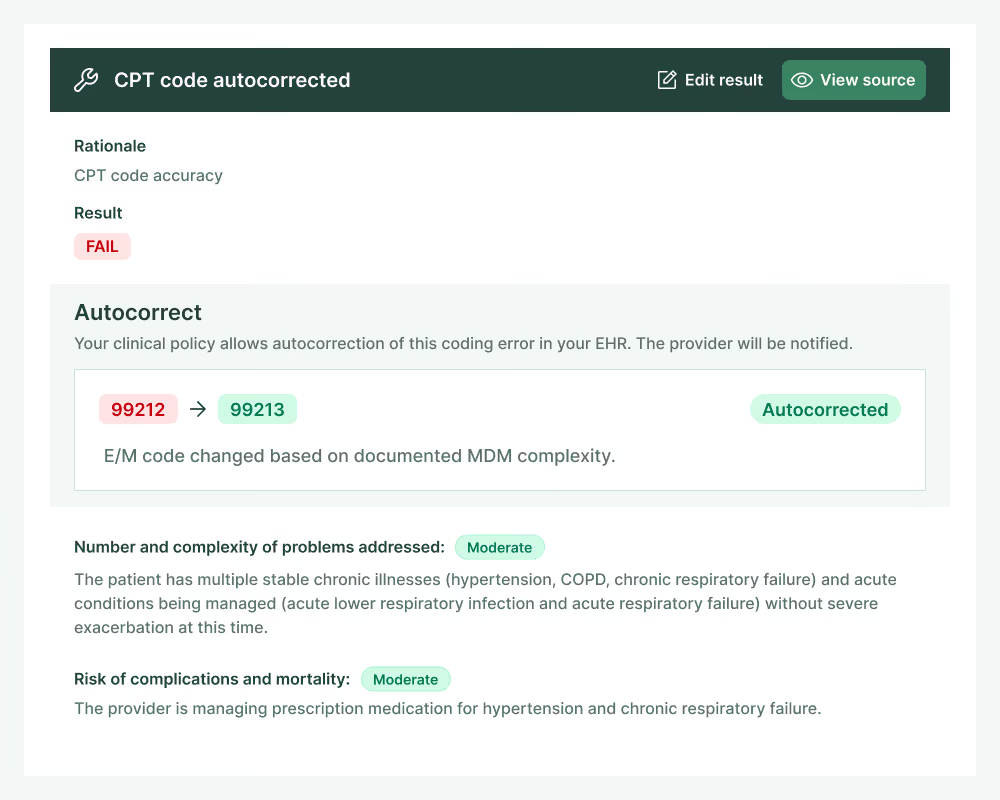
Charta detects and corrects missed revenue opportunities by ensuring you code every service delivered, and verifies that E/M codes are billed at the highest defensible level.

By catching coding errors and documentation gaps pre-billing, Charta shifts your compliance strategy from reactive to proactive. Address issues while charts are still open, eliminating preventable denials and audit exposure.

Comprehensive analysis of every encounter gives clinical leaders actionable data on supporting quality measures, identifying care gaps and improving documentation quality. Automated feedback loops help providers improve in real-time, raising the quality of care and clinical records simultaneously.

Charta's AI analysis identifies missed opportunities supported by clinical documentation, providing reviewers with direct citations to accelerate validation. The result: higher accuracy, faster turnaround, and reduced cost per chart reviewed.

Charta reviews all documentation immediately after note submission to completely and accurately code every service.
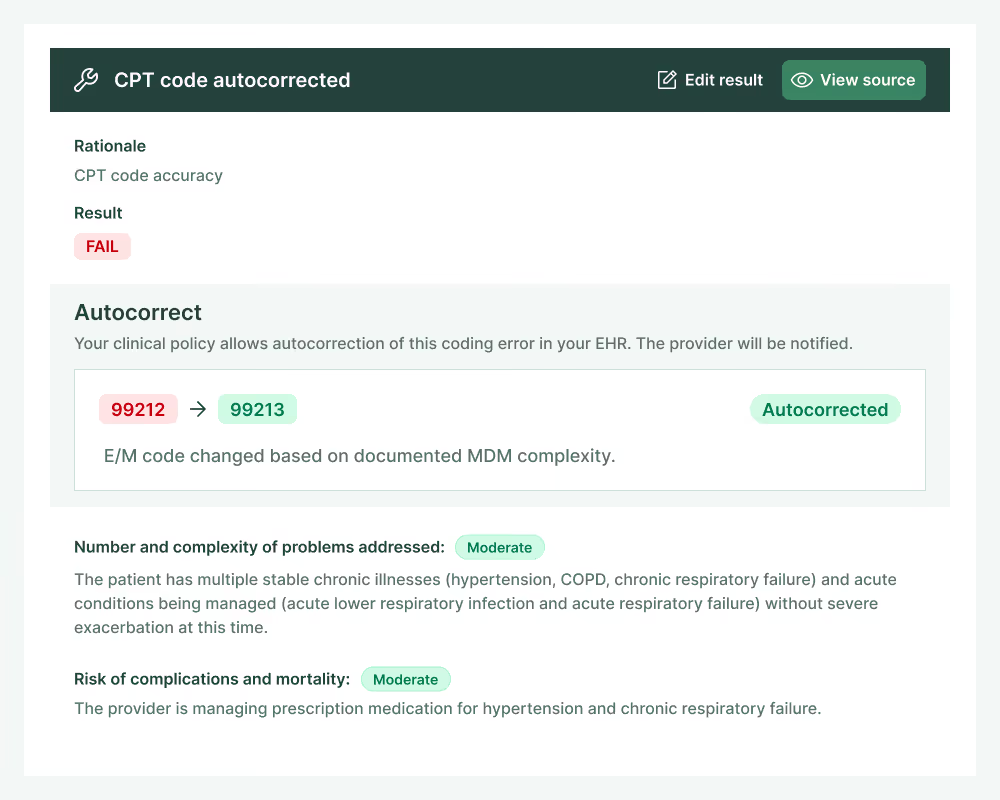
Charta detects and corrects missed revenue opportunities by ensuring you code every service delivered, and verifies that E/M codes are billed at the highest defensible level.
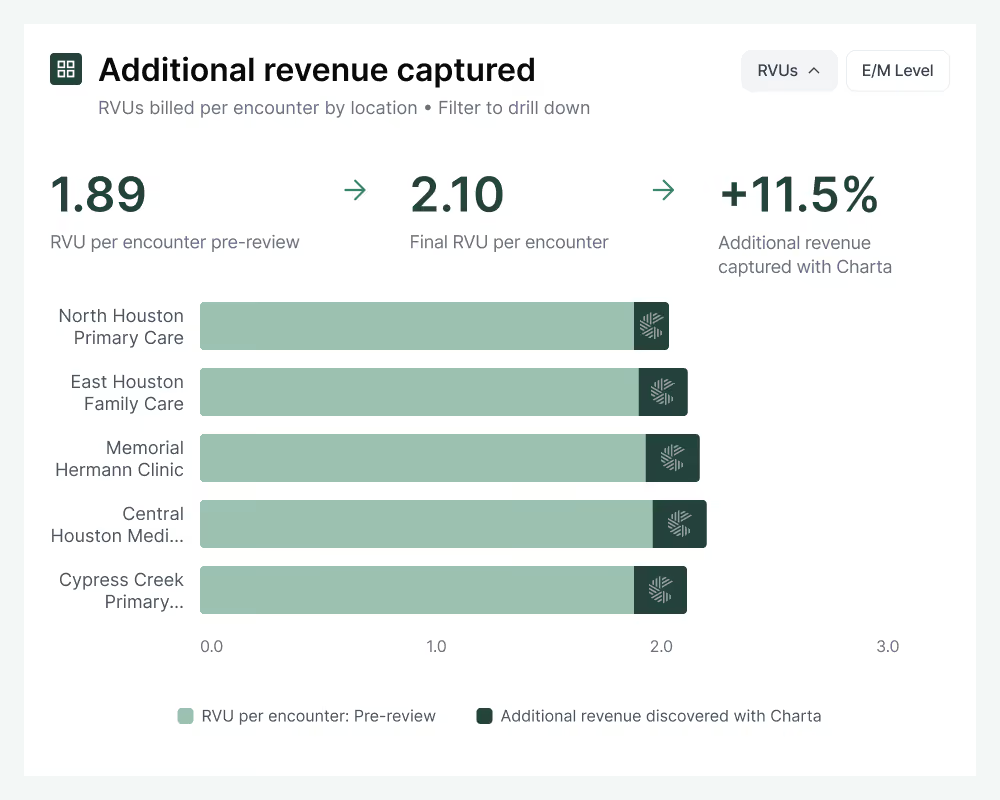
By catching coding errors and documentation gaps pre-billing, Charta shifts your compliance strategy from reactive to proactive. Address issues while charts are still open, eliminating preventable denials and audit exposure.

Comprehensive analysis of every encounter gives clinical leaders actionable data on supporting quality measures, identifying care gaps and improving documentation quality. Automated feedback loops help providers improve in real-time, raising the quality of care and clinical records simultaneously.
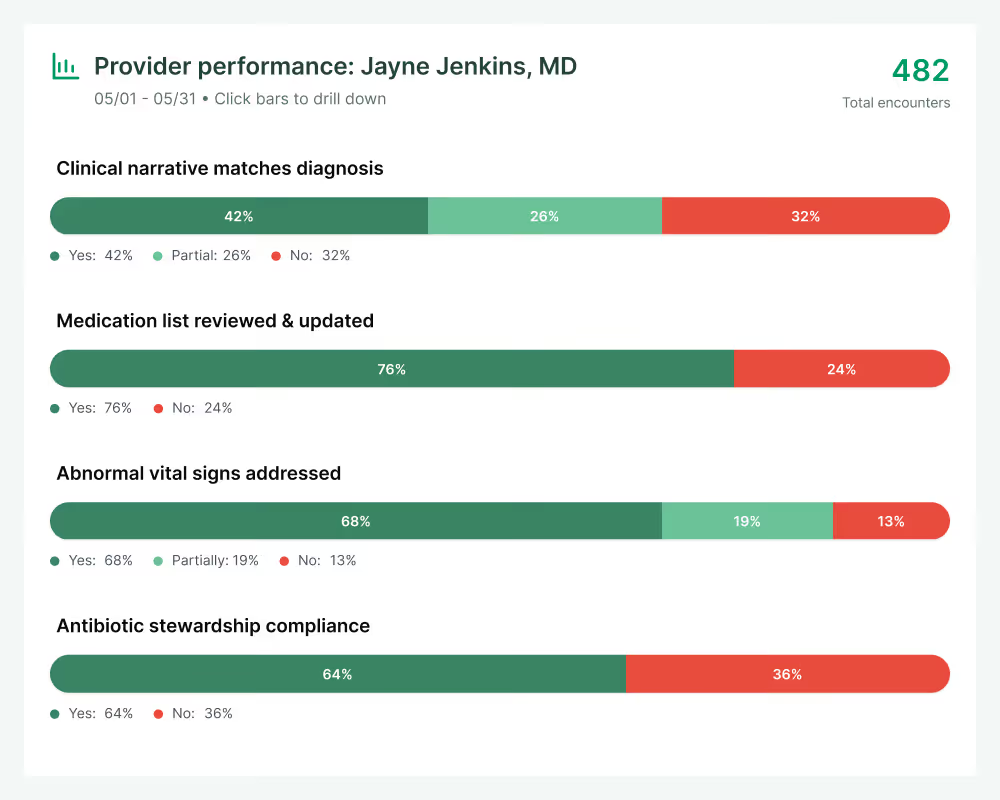
Charta's AI analysis identifies missed opportunities supported by clinical documentation, providing reviewers with direct citations to accelerate validation. The result: higher accuracy, faster turnaround, and reduced cost per chart reviewed.